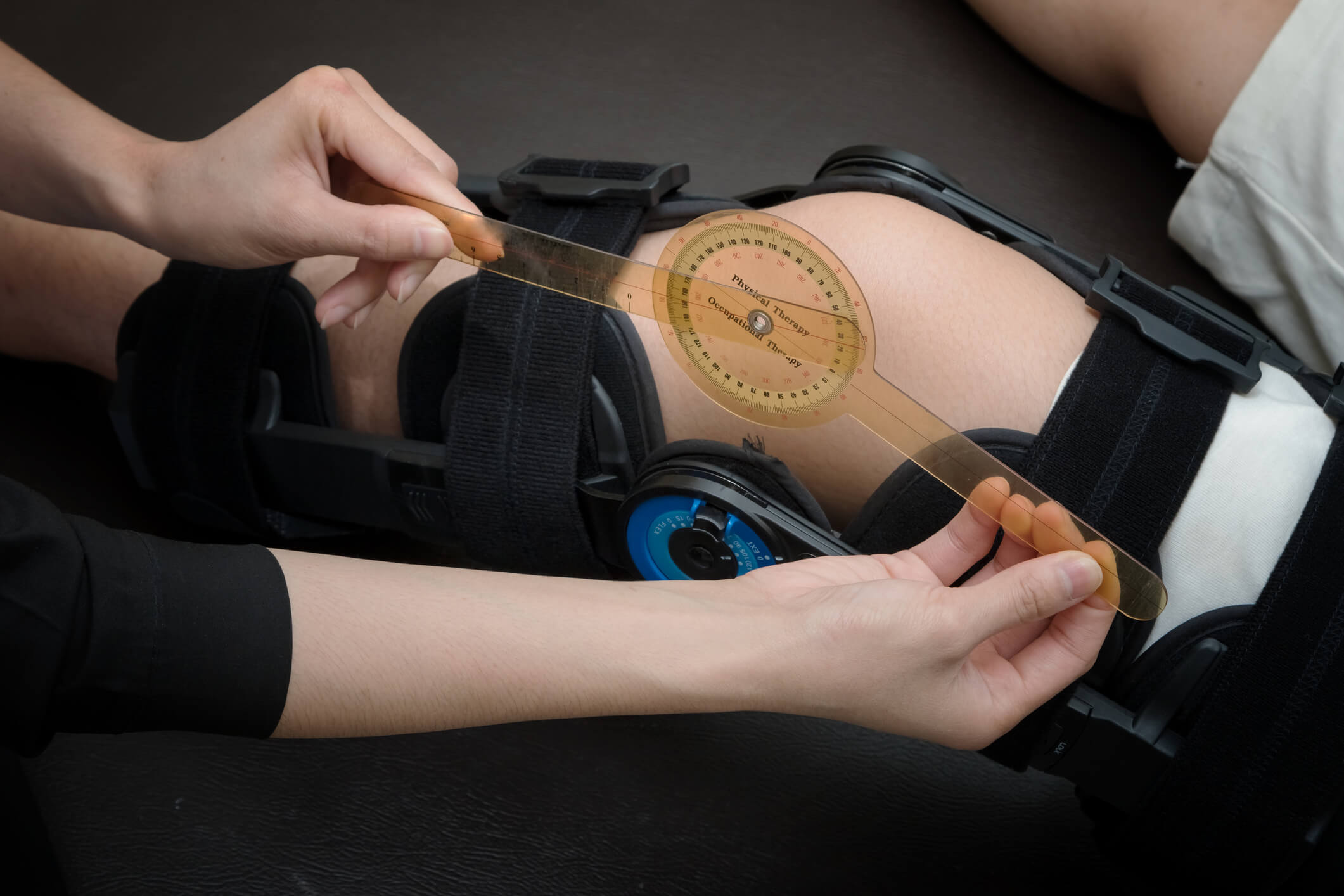
Accidents happen. We’re here to help you.
When an employee is injured on the job, KEMI is ready to help you navigate the claim process and provide the highest standard of care available to the claimant throughout the claim. Learn how KEMI helps you manage claims, check out our frequently asked questions, or contact us if you have specific claims questions.



Report an incident or illness immediately.
Guide the claimant on seeking initial medical treatment.
Provide KEMI with requested wage information.
Take corrective action if possible to prevent future incidents.
Submitting a First Report of Incident
Submit the First Report of Incident or Illness online for the quickest and easiest way to report a claim.
A claim may also be reported by:
- Email – complete First Report of Incident or Illness (IA-1 form) and email to claim@kemi.com.
- Fax – complete the First Report of Incident or Illness and fax to 859-425-7822.
- Phone – call 800-640-KEMI (5364) during business hours Monday – Friday from 8 a.m.-5 p.m. Eastern time.
- Mail – print and complete the First Report of Incident or Illness and mail to:
KEMI
ATTN: Claims Unit
P.O. Box 12500
Lexington, KY 40583-2500
The Claims Process
Once an incident is reported to KEMI, our Claims Team will move into action by reviewing the information and ensuring the claimant receives the appropriate care. Reporting the claim isn’t just good practice, it’s the law. KRS 342.038 requires policyholders to report injuries or illnesses to us within three working days of receiving notification of the incident or alleged incident.
Once we’ve reviewed the First Report of Incident, we will request additional information from you as we determine appropriate benefits for the claimant. If the claimant needs ongoing treatment, please refer the individual to our Managed Care Network. If the claimant is able to return to work with restrictions, we will work with the you to make those accommodations if possible.
As part of our commitment to you, we want to help your employee return to work as quickly and safely as possible.
Resources for Employers
KEMI works closely with the Occupational Managed Care Network (OMCA) to provide quality care for work-related injuries.
KEMI has partnered with Medcor to provide you with an extra level of service when workers’ compensation claims arise.
Both policyholders and claimants benefit from KEMI’s extensive claims management tools and resources. These resources include a pharmacy benefit management (PBM) program to monitor prescription drug trends and a medical bill review program to identify duplicate billing and coding errors.
Quick Links:
Additional Resources
The following resources highlight several of the benefits policyholders receive when choosing KEMI for their workers’ compensation coverage.
Claims Detail Dashboard
Policyholders may log in to access important claims details using our interactive Claims Detail Dashboard.
log in or registerManaged Care Network
KEMI’s Managed Care Network through OMCA provides claimants with quality care.
Learn about Managed CarePharmacy Benefits Manager
Our PBM program by Mitchell helps control prescription costs, which helps lower the overall premium of the policy.
How We control Rx CostsMedical Bill Auditing
Our Medical Bill Team makes sure provider services are adjusted to the fee schedule and paid appropriately.
Learn about our processLoss Control & Safety
Our Claims Team works closely with our Loss Control & Safety Team to investigate and prevent injuries.
ACCESS FREE SAFETY RESOURCESMedcor
KEMI has partnered with Medcor to provide you with an extra level of service when claims arise.
Register for medcorKEMI has a zero-tolerance policy on workers’ compensation fraud to protect our policyholders and their employees. Report fraud.
Claims Forms
- IA-1 First Report of Incident
- Direct Deposit
- Direct Deposit (Spanish)
- Average Weekly Wage Certification (AWW)
- Medical Waiver & Consent Form (Form 106)
- Notice of Designated Physician (Form 113)
- Claimant Reimbursement Form (Form 114)
- Job Analysis Form
- W-9 Taxpayer Identification Number Request Form (IRS Website)
Still have questions?
If you have a claims question, give us a call at 1-800-640-KEMI (5364) or 859-425-7800. You may also use the contact form here.