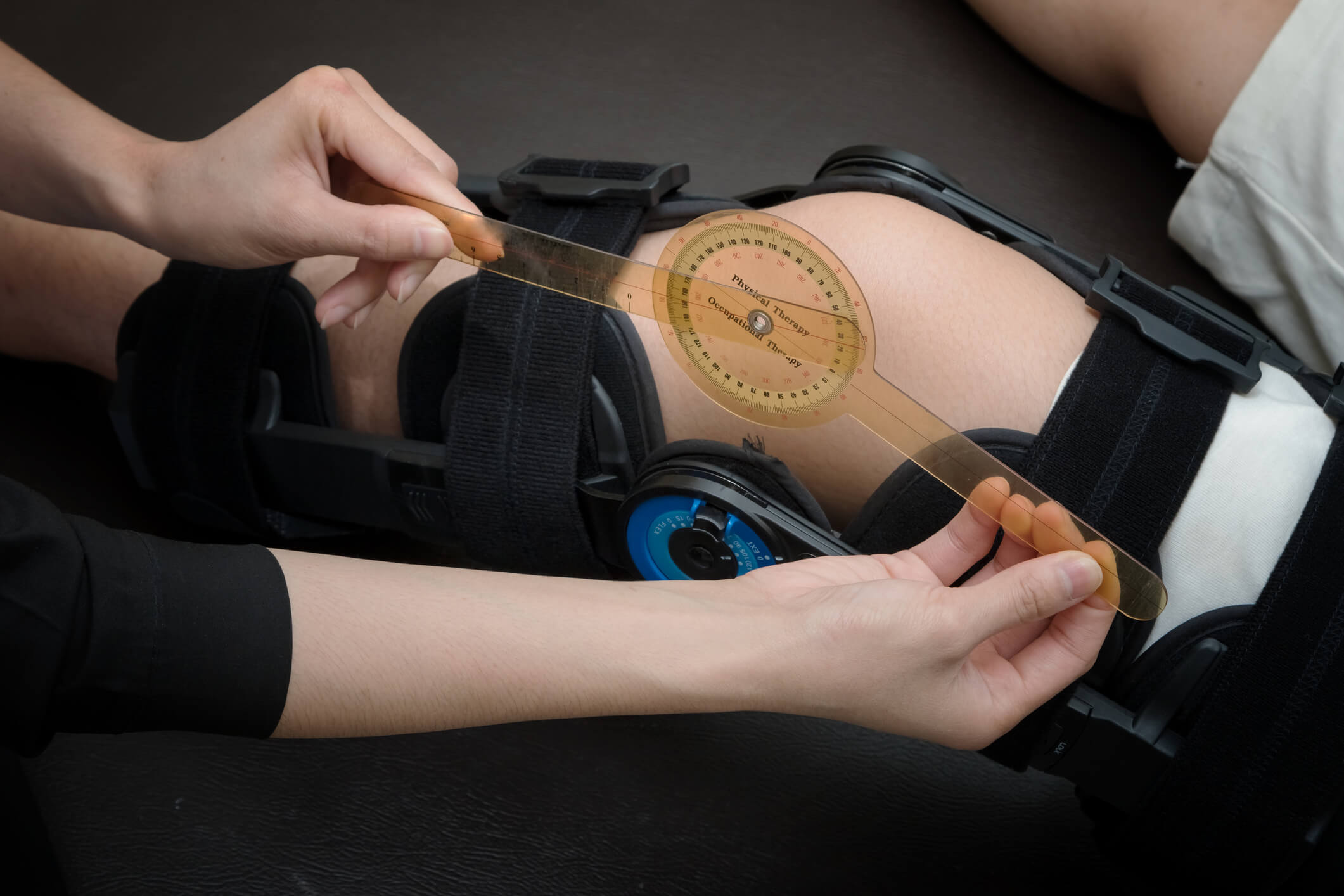
KEMI’s Medical Bill Team combines internal and external expertise to make sure the services received by injured workers are billed to KEMI correctly.
We reference Kentucky’s fee schedule and cost-to-charge ratio before sending bills on to be reviewed and approved by KEMI examiners, and we also make sure services are paid in a timely manner.
As a result, each year KEMI saves millions of dollars by identifying and preventing payment on duplicate bills, overcharges, or other billing errors. By controlling our medical expenses, KEMI is able to pass these savings on to our policyholders as we determine future rates.

Claims Resources for Employers
The following resources highlight several of the benefits policyholders receive when choosing KEMI for their workers’ compensation coverage. For information on other resources available for policyholders, contact us today.
Claims Detail Dashboard
Policyholders may log in to access important claims details using our interactive Claims Detail Dashboard.
log in or registerManaged Care Network
KEMI’s Managed Care Network through OMCA provides claimants with quality care.
Learn about Managed CarePharmacy Benefits Manager
Our PBM program by Mitchell helps control prescription costs, which helps lower the overall premium of the policy.
How We control Rx CostsMedical Bill Auditing
Our Medical Bill Team makes sure provider services are adjusted to the fee schedule and paid appropriately.
Learn about our processLoss Control & Safety
Our Claims Team works closely with our Loss Control & Safety Team to investigate and prevent injuries.
ACCESS FREE SAFETY RESOURCESMedcor
KEMI has partnered with Medcor to provide you with an extra level of service when claims arise.
Register for medcorKEMI has a zero-tolerance policy on workers’ compensation fraud to protect our policyholders and their employees. Report fraud.